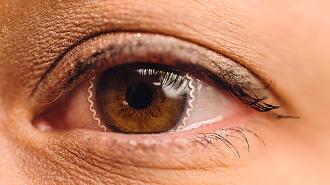
There’s a certain insidiousness to the way glaucoma — a group of eye diseases that damage the optic nerve — can snatch away a person’s vision.
That damage can be so slow that people may never notice until it is too late, and the long term impacts, like loss of peripheral vision, blind spots, and blindness, have set in.
Glaucoma impacts tens of millions of people globally, and is the second leading cause of blindness, after cataracts. Now, Purdue University researchers have developed smart contact lenses that may help save people’s sight.
Glaucoma can steal sight so slowly people may not notice.
Keeping an eye on it: The best way to ward off vision loss is through regular eye examinations and early detection, where eye doctors check on five factors: the pressure inside the eye, your field of vision, the shape and color of the optic nerve (this is why you’re dilated), and structural tests looking at the angles and thickness of different eye structures.
That first one is key: according to Purdue researchers, the pressure inside your eye — called intraocular pressure, or IOP — is the only risk factor that can be modified.
A device called a tonometer determines IOP by measuring how much force is needed to flatten an area of the cornea. At the eye doctor, this is usually done with pressure applying devices (either hand held or in a machine) or the air-puff test.
The problem: The problem is, a tonometer has its limits.
You can have an eye doc do it, sure, but visiting a clinic “remains a significant burden and also has become a particular challenge throughout the ongoing global pandemic,” the researchers wrote in their study, published in Nature Communications.
Current at home tonometers allow for patients to measure IOP, but wearable ones often have thick, uncomfortable lenses, and readings during sleep are unobtainable “due to the requirement of patients to stay awake during measurements,” the authors noted dryly.
The pressure inside your eye is the only glaucoma risk factor that can be modified.
“The largest increase in IOP often occurs while people are lying down, when overnight IOP is typically 10% to 20% greater than daytime IOP,” Purdue biomedical engineer Chi Hwan Lee said.
“Vision loss may occur during sleep without the patient noticing it, even if daytime in-clinic or at-home measurements indicate normal IOP.”
Being able to get continuous IOP data could be key to catching glaucoma as early as possible.
A 24-hour tonometer: Lee and his colleagues at the Indiana University School of Optometry and Johns Hopkins turned to Lee’s specialty: “sticktronics” — sticker-like devices with electronics and smart tech embedded in them.
“[W]e developed a unique class of smart soft contact lenses built upon various commercial brands of soft contact lenses for continuous 24-hour IOP monitoring, even during sleep at home,” Lee said.
The smart lenses have all the usual features of commercial leave-in contacts, features that current wearable tonometers lack and will be important for people actually using them.
“This tonometer is significantly more comfortable than any other type of contact lens sensor we have come across and more comfortable than any currently available commercially available IOP sensor,” said Pete Kollbaum, a study author and professor and associate dean for research at Indiana University School of Optometry.
Smart contact lenses that measure eye pressure 24/7 could help catch glaucoma.
How it works: Using the commercial lenses — with their tried-and-true safety profiles and comfort features — as a base, the team added a soft, thin, stretchy tonometer. Resembling a gentle waveform ringing the lens, the tonometer measures IOP by stretching or compressing based on the curvature of the eye, which changes with IOP.
Those measurements are sent wirelessly with a low-power signal to a pair of smart glasses or a sleep mask. That 24-hour IOP data can then be shared with doctors using an encrypted server. The tonometer can also issue an alert signal if it detects IOP elevation worthy of a clinical visit.
The device was evaluated in dog, rabbit, and human eyes to check its accuracy and wearability. Lee and colleagues suggest further clinical trials in glaucoma patients with different conditions, like dry eye disease and those who have had a glaucoma surgery.
They also see the tech being adaptable to studying other eye problems.
“The eye is a very challenging body part that is even softer, more sensitive and curvilinear when compared to the skin,” Lee said. “We hope our approach can be also tailored for aiding and detecting other chronic ocular diseases and for other functions.”
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].