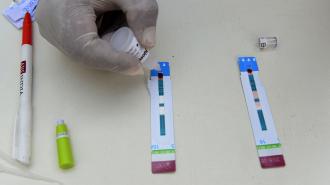
As the COVID-19 pandemic has shown the feasibility of home testing, some public health experts and lawmakers have finally begun a push to encourage home testing for sexually transmitted infections, in the hopes of curbing soaring rates of STIs.
CDC data for 2020 captures that upward trend: gonorrhea cases were up 42% compared to 2016, syphilis up 52%, and congenital syphilis — syphilis passed on during pregnancy — rose a staggering 235%, with 2,148 cases and 149 stillbirths and infant deaths.
As the pandemic has shown the feasibility of home testing, some public health experts and lawmakers have finally begun a push to encourage home testing for sexually transmitted infections.
All of which seems worse considering these numbers are likely an undercount — and the pandemic redirected STI surveillance resources and cut down in-clinic visits, as Nature’s Carrie Arnold pointed out.
But home testing could help offset that, with new laws being passed to require insurance coverage of home testing and new STI tests being approved.
“I think we’ve all become more comfortable self-testing with COVID,” Natalie Cramer, of the National Alliance of State and Territorial AIDS Directors, told Nature. “It’s opened up both a need and a comfort level that folks have around it.”
New laws, new tests: California was the first state to pass a law requiring health insurers to cover home tests for STIs, going into effect this past January.
“This is the first law of its kind, and I’d say it’s kind of cutting-edge,” Stephanie Arnold Pang, senior director of policy and government relations for the National Coalition of STD Directors, told the Los Angeles Times. “We want to bring down every single barrier for someone to get STI testing, and out-of-pocket cost is a huge factor.”
In April, the Colorado Department of Public Health (CDPH) began offering free STI self-testing kits, mailed discreetly to people’s homes. The state suffers from the same increase in STIs as the nation, and officials hope that the new program can tear down another barrier to testing: stigma.
“Some would prefer to be tested at home confidentially, or may not have a medical home where they could go, and so we are seeing more and more opportunities for at-home tests,” Eric France, the CDPH’s chief medical officer, told Denver’s Fox 31.
STI rates have been increasing.
There are a suite of at-home tests already available, Nature reported. In 2012, the FDA finally approved an at-home HIV test (26 years after the first at-home test was developed). Syphilis self-tests, which use small drops of blood or swabs, arrived in the late 2010s.
Tests that cover a variety of STIs in one go are coming, as well.
Abbott received the go-ahead from the FDA for their new test, which looks for cervicitis, chlamydia, gonorrhea, trichomoniasis, and urethritis using only a single swab or urine samples. The test’s versatility could help give doctors a better picture of a patient’s health and develop the proper treatments for them faster, Abbott’s Kathryn Becker told FierceBiotech. But it is currently only approved for samples gathered in clinical environments, even if the patient is the one doing the sampling themselves.
Abbott plans to move into at-home testing next, Becker said, the value of which was proven in the pandemic.
“As we look to the future of testing, we will be focused on bringing that kind of convenience and discretion for STIs and other conditions,” Becker said.
The limitations of at-home testing: While clearly helpful for patients, at-home testing does have drawbacks.
Chief among them is that tests are only as effective as the samples they are testing from, samples that must be properly gathered and applied to the test media.
Home results also may not become important data points for public health officials, University of Alabama at Birmingham gynecologist Shweta Patel told Nature. The onus is on the user to not only report their own results, but also perform their own contact tracing — something she said does not always happen.
Testing samples collected at home in labs can increase their accuracy, but time is also a factor, as we learned in the pandemic. Syphilis tests that send samples in to a clinic or lab can have true negative and true positive rates over 98% when used correctly, Nature reported, but they can take weeks to return results, limiting their effectiveness as public health tools.
Empowering individuals to know their own status could prove to be an important aspect of the response.
The cost of tests — which can run from $40 to over $100 — may be one reason why the ones already approved are not more popular (something the California law seeks to address). Clinical tests have also found result discrepancies among different users and different lots of the tests, Nature reported.
Still, with STIs on the rise, including superbugs like drug-resistant gonorrhea, empowering individuals to know their own status could prove to be an important aspect of the response.
“We have children born in California with syphilis,” California state Senator Richard Pan, who wrote the STI testing law, told the LA Times.
“You’d think that went away in the Victorian era.”
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].