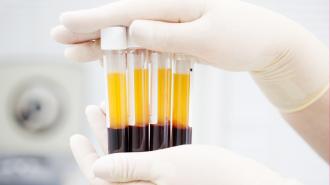
The Japanese pharmaceutical company Takeda hopes to make the world’s first drug treatment for COVID-19 using the blood plasma of people who’ve already fully recovered from the respiratory disease.
“These are patients who have healthy immune systems,” Chris Morabito, head of research and development at Takeda’s plasma-drug business, told the Wall Street Journal. “They’ve recovered from it. They generated the antibodies. Those are permanent, and we want them. We want to use them as a drug.”
How Can Blood Plasma From Coronavirus Survivors Help?
When an antigen — a bacteria or a virus, such as SARS-CoV-2 — enters the body for the first time, the immune system responds by producing an antibody, a protein designed to bind to that specific antigen. This lets other cells in the immune system know to destroy the intruder.
After the body completely clears out the antigen, the antibodies for it remain in the body. If that specific antigen ever invades again, the immune system can react to it even more quickly — it doesn’t have to go through the process of producing the antibody from scratch again.
Takeda’s therapy could work alongside vaccines, antiviral drugs, and other treatments.
Antibodies can be found in blood plasma, the liquid part of blood. More than a century ago, during the Spanish flu pandemic, researchers realized that injecting plasma from someone who’d recovered from the flu improved the likelihood that a person with a severe case would survive.
Takeda has been developing plasma-based products for more than 75 years, and on March 4, it announced plans to test whether doctors could use any of its existing products to treat COVID-19 patients.
It also said it plans to begin developing TAK-888, a new plasma-based therapy designed specifically to address the novel coronavirus.
To that end, Takeda is now looking to source blood plasma from coronavirus survivors and discussing how best to expedite the development of TAK-888 with health officials in the U.S., Asia, and Europe.
Collective COVID-19 Response
Even if Takeda succeeds in the development of TAK-888, though, it’s unlikely to single-handedly bring the COVID-19 outbreak to an end.
For one, there’s a problem of scale. As Julie Kim, the president of Takeda’s blood plasma unit, told STAT, a blood plasma donation from a coronavirus survivor would likely only produce enough treatment for one patient — and it’s possible Takeda will need to use plasma from several donors for each patient.
“We are not looking at this as a therapy that everyone should go on,” Kim told STAT. “This will be targeted to patients who have severe disease.”
Still, until someone develops a vaccine or drug treatment for COVID-19, the most doctors can do is provide patients with supportive care and hope their bodies are able to fight the infection.
Thankfully, more than 35 other companies are simultaneously scrambling to develop drug-based COVID-19 treatments, and Takeda’s blood plasma approach could work alongside vaccines, antiviral drugs, and other treatments to help bring an end to the COVID-19 outbreak.
“We need them all,” infectious disease expert Greg Poland told STAT.