When CRISPR Therapeutics and Vertex used gene editing to try to cure heritable blood disorders in 2019, it marked the first CRISPR trial outside of China.
A year later, the trial — using the CRISPR gene editor to treat sickle cell disease and beta thalassemia — showed promising results, Freethink reported in 2020.
Now, three years after the trial began, the researchers have presented new data showing that the treatment continues to be effective.
“These data provide further evidence that this treatment has the potential to be transformational for patients with sickle cell disease and beta thalassemia,” trial abstract author Stephan A. Grupp of the Children’s Hospital of Philadelphia said in a statement.
New data shows that the CRIPR sickle cell and beta thalassemia treatment continues to be effective even three years out.
The diseases: Severe sickle cell disease (SCD) and transfusion-dependent beta thalassemia (TDT) are both caused by genetic mutations impacting hemoglobin, the molecule red blood cells use to carry oxygen throughout the body.
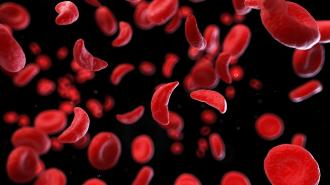
In SCD, atypical hemoglobin causes the red blood cells to twist out of shape, contorting into crescents — or sickles — that cannot deliver oxygen as well. The disease can cause tiredness and shortness of breath, and periodic sickle cell crises cause intense pain.
In TDT, patients do not produce enough hemoglobin at all, sometimes requiring repeated blood transfusions, which have their own risks and side effects.
Both can be treated by a stem cell transplant from a suitable donor, which not only requires finding a good match but may also require suppressing the patient’s immune system.
The therapy: The CRISPR treatment, originally dubbed CTX001 and now called exa-cel, is a one-time treatment that genetically alters the patient’s own cells to produce the kind of hemoglobin found at birth, which isn’t distorted, allowing red blood cells to work properly.
The new data, presented at the European Hematology Association Congress but yet to be published in a peer-reviewed journal, reported results from 75 patients.
Of the TDT patients, 42 out of 44 were blood transfusion-free up to 37.2 months after their exa-cel infusion, according to CRISPR Therapeutics and Vertex. They are essentially cured of the disease.
The CRISPR therapy is a one-time treatment that genetically alters the patient’s own cells.
The remaining two patients needed much less transfusion volume, and all of the TDT patients had elevated levels of fetal hemoglobin and total hemoglobin in their blood.
All of the SCD patients were free from sickle cell attacks, up to 32.3 months later.
Two of the TDT patients suffered adverse effects possibly related to exa-cel, including delayed growth of white blood cells and a low blood platelet count, both of which resolved on their own.
Importantly, the team found no evidence of exa-cel’s effectiveness waning over time, even three years after infusion.
“Although we must continue to investigate the durability of these results, I am excited about the current data,” Grupp said.
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].