Forever is what separates the tattoo from other forms of art. Permanence — and pain — are the medium and the promise; that what you are getting is essentially indelible, etched into your very skin and as a part of you as the canvas it rests within.
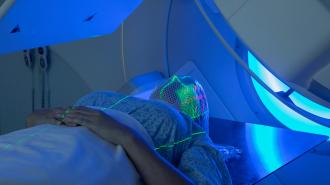
But people at Michigan’s Henry Ford Health have begun testing tattoos that are destined — and designed — to disappear. With made-to-fade ink maker Ephemeral Tattoo, the researchers have begun a trial to test the safety and efficacy of non-permanent tattoos for cancer patients undergoing radiation therapy.
Tattoos are often used to help guide radiation treatment. But patients may resist traditional tattooing because of religious or cultural reasons, or because they dread a reminder of their cancer, while non-permanent options, like henna or various other temporary tattoos, can fade too quickly and fail to last for the duration of treatment.
“We believe semi-permanent tattoos could offer patients an alternative to permanent tattoos, which has long been the standard of care for radiation therapy alignment,” Eric Schaff, a radiation oncology resident at Henry Ford Health who initiated the study, said.
Tattoos are often used to help guide radiation treatment. But patients may resist traditional tattooing because of religious or cultural reasons, or because they dread a reminder of their cancer.
Precision therapy: In radiation therapy, high doses of intense energy are used to kill cancer cells and shrink tumors. It’s a common form of treatment, with roughly 50 to 60% of cancer patients receiving some form of it, Schaff tells Freethink, either to cure the cancer or help manage symptoms.
The radiation beams damage the DNA within malignant cells; when enough damage is done, the cells eventually die and are removed from the body. Radiation therapy can also damage healthy cells, so modern methods come down to precision — hitting the target as accurately as possible, while minimizing the amount of radiation hitting healthy tissue.
“With advances in radiation technology, we’re much more precise than we used to be,” Schaff says. Each radiation therapy course is different, designed for a particular cancer patient, and delivered with an accuracy down to a few millimeters at the least, Schaff says.
“So now, patient alignment is as important as ever,” for effective therapy that keeps healthy cells safe, Schaff says.
To ensure the targeting is correct every time over the course of weeks, small dots — most typically three, Schaff says — are tattooed with a hypodermic needle as setup points.
Non-permanent options like henna or other temporary markings may fade before the therapy is done. Ephemeral’s ink is designed to last the entire course, then disappear.
The problem with permanency: For many patients, the tattoos are just part of the process, something that has to be done to win, like surgery or chemo.
“Once we’ve talked to them, once we’ve explained to them, once they’ve overcome their initial shock of ‘oh, I need a tattoo, I need a permanent reminder of my treatment’ … most patients are quite understanding,” Farzan Siddiqui, a radiation oncologist at Henry Ford Health and the trial’s principal investigator, tells Freethink.
But for others, they can be a burden in an already difficult time and a source of angst. Patients may be scared of the needle and the pain. Breast cancer patients may worry about having their “battle scars” revealed in various outfits, Siddiqui offers as an example. Others may have religious or cultural traditions that consider tattoos taboo; parents may worry about their young children receiving life-long reminders of it.
Obvious work-arounds like henna or other temporary tattoos often do not last long enough for an entire radiation therapy course, which can take weeks, Schaff and Siddiqui say. Every new alignment means another chance to potentially be those few millimeters off, and needing to be realigned makes visits longer and keep other patients waiting.
The team wanted to find a solution that is not a permanent reminder, and would not conflict with faith or cultural values, Siqqidui says.

Out, damned spot: In the trial, 15 radiation therapy patients received a total of 44 tattoos with Ephemeral’s made-to-fade ink. The study was designed to test the safety and tolerability of Ephemeral’s ink, as well as if it would last the entire treatment — but then, importantly, fade away. Henry Ford Health’s diverse patient population helped to ensure a trial with an array of skin tones, a factor that comes into play when talking tattoos.
It took years of research to create an ink designed to last for a while but then purposefully fade away; the work began in 2014, and improvements are still being made, Ephemeral co-founder and chief technology officer Brennal Pierre tells Freethink.
“We needed something that would break itself down,” Pierre says of the challenge.
Pierre and colleagues turned to combining materials they already knew were biodegradable with proven-safe color additives. The ink is made from medical-grade polymers — like the kinds which comprise dissolvable stitches, Pierre says — as well as natural and synthetic color additives regularly used to give a hue to food, drugs, and cosmetics. Eventually, the ink breaks down enough in the body that the immune system carries it away.
Tattoo trials: It took multiple iterations to find an ink formula that will last through radiation therapy then fade away in a reasonable time; these are unique challenges different from recreational tattoos, so the ink must be optimized for its new job. Trial data can help dial this in by finding real-world variables that may be missing in a lab setting.
“If this is going to become a standard treatment, we want to make sure we understand all of the variables involved,” Pierre says.
The tattoos were given to patients with a normal tattoo machine, rather than the more painful hypodermic needle. There were no adverse effects among the patients, and the ink lasted the entire course of their radiation therapy.
The study is now in a longitudinal arm to assess how well, and how fast, the tattoos are fading. As they come back to Henry Ford for their regular checkups, patients will have photos taken of their dots and be recorded on a visibility scale from one to four.
The furthest patient out at this point is around six months out, Schaff says, so the jury’s out on the fade aspect of the study. He has given himself dots with Ephemeral Ink, however, and can see it fading.
Henry Ford Health radiation oncology resident Eric Schaff, who initiated the trial, has given himself dots with Ephemeral Ink, and can see them fading away.
So, too, can study patient Delores Miller. “I can barely see it,” Miller, who received radiation therapy following her breast cancer surgery, tells Freethink. “So it’s just about gone.”
(While Miller has not officially been examined for fading yet, Schaff says that he would expect hers to be fading by now based on prior experience with the ink.)
Miller had no qualms at the idea of getting a tattoo; it was necessary for her treatment, and being rigorous in your therapy, listening to your doctors, and doing what needs to be done is important, Miller says. But they liked the idea of testing Ephemeral’s made-to-fade ink to help future patients.
“I can understand people not wanting it for religious reasons, but it’s necessary,” Miller says.
The researchers will continue to follow patients for at least a year, to assess how well the tattoos fade away, and plan to do a peer-reviewed paper as they attempt to see if temporary tattoos could be a new standard of care.
“I think the technology is going to really help people out,” Schaff says.
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].