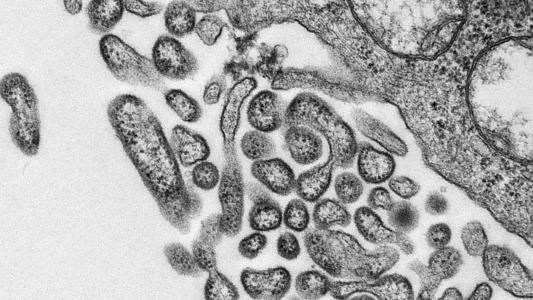
As many as 50 perfectly healthy adults in the U.K. may soon expose themselves to the coronavirus — for science.
The study is called a human challenge trial, and its purpose is to speed up our understanding of the disease and the efficacy of vaccines. By deliberately exposing a few dozen volunteers, researchers can get results immediately, without having to vaccinate tens of thousands of people and wait for some of them to encounter the disease naturally.
Experts have been contemplating the benefits of a human challenge trial for COVID-19 since nearly the beginning of the pandemic, but deliberately exposing people to a new, potentially deadly virus is fraught with controversy, to put it mildly.
Yet nearly 40,000 people, from almost 170 countries, have already signed up to volunteer for it, according to the grassroots advocacy group 1 Day Sooner, which advocates for COVID-19 challenge studies.
Now, the U.K. has agreed to invest $44 million in what will be the world’s first human challenge trial for COVID-19 — assuming researchers secure final regulatory and ethical approvals before the planned January start date.
Human Challenge Trial for COVID-19
The U.K’s human challenge trial for COVID-19 is a collaboration between the government, Imperial College, Royal Free London NHS Foundation Trust, and hVIVO, a company with experience conducting viral challenge studies.
The project will consist of two phases.
The first phase will involve up to 50 volunteers between the ages of 18 and 30 who haven’t already contracted COVID-19. The volunteers will have no underlying health conditions and no risk factors for the disease (diabetes, obesity, etc.). The CDC estimates the risk of dying for this group to be extremely low, so they are considered the safest group for a challenge trial.
The goal of this phase is to determine the smallest amount of the coronavirus needed to cause an infection (something we still don’t know, eight months into the pandemic), so it’ll start with exposing the volunteers to a tiny amount of the virus.
There’s the possibility here of putting people at risk without much of an upside.
Jeremy Faust
If no one contracts COVID-19, they’ll increase the amount incrementally until it causes an infection.
The researchers will then study the infected volunteers to see how much of the virus they release into the environment (by breathing, coughing, etc.) — this will hopefully help us better understand how the coronavirus spreads and for how long.
The volunteers will stay at a study facility for the entire process and won’t be allowed to leave until they test negative for COVID-19 in two highly sensitive tests. They’ll be paid for their time (likely around $5,000).
If the first phase goes well, a second phase will follow. It’ll focus on testing the efficacy of different coronavirus vaccines and treatments on up to 500 volunteers.
Worth the Risk?
The possibility of a human challenge trial for COVID-19 has prompted a variety of responses from the scientific community.
In July, over 100 top scientists and ethicists, including 15 Nobel Prize winners, signed a letter urging the NIH to conduct COVID-19 challenge trials, arguing that these studies can guide research and accelerate improvements in vaccine design.
A public opinion study in eight countries also found broad public support for the idea, with 75% of participants endorsing the trials, even while acknowledging the risks.
“This high support is consistent across every geography and demographic subgroup we examined,” the study authors concluded, “including people of diverging political orientations and vulnerable populations such as the elderly, essential workers, and racial and ethnic minorities.”
The benefit could be possibly saving people’s lives.
Seán McPartlin
Others argue that a human challenge trial for COVID-19 simply isn’t worth the risk.
“Given that we may have an approved vaccine in the coming months, I don’t know how much challenge studies would speed along the process,” Jeremy Faust, a Boston-based emergency medicine physician, told CNBC. “There’s the possibility here of putting people at risk without much of an upside.”
Still, thousands of people, including Seán McPartlin, a 22-year-old student at the University of Oxford, say they’re willing to take on the risk of deliberate infection right now.
“Even if the long-term effects turn out to be even worse than what we suspect, I still think there are many volunteers — including myself — who would be willing to go ahead because the benefit could be possibly saving people’s lives,” he told the Guardian.
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].