MRI-guided focused ultrasound — a technique that uses vibrating “microbubbles” to create gaps in the blood-brain barrier — has been used to try to treat brain cancer in children for the first time. If it works, the novel technique could help thousands of children facing these deadly diseases.
The challenge: Diffuse intrinsic pontine glioma (DIPG) is a rare, highly aggressive type of pediatric brain cancer — even with treatment, the median survival time after diagnosis is less than a year. The cancer starts in the pons, a critical area of the brainstem responsible for breathing, heart rate, and other vital functions.
Only about 10% of patients with DIPG will survive two years after diagnosis.
The location makes the tumors inoperable, and chemotherapy isn’t typically effective, due to the blood-brain barrier. The barrier is designed to keep pathogens and toxins out of the brain, but it also makes it extremely difficult to get medications into the brain.
Radiation therapy can temporarily slow the progression of DIPG, but even with radiation, only about 10% of patients will survive two years after diagnosis.
What’s new? In 2015, researchers at Toronto’s Sunnybrook Health Sciences Center demonstrated a way to use focused ultrasound waves to temporarily open the blood-brain barrier, increasing the passage of chemotherapy into the brain of an adult cancer patient.
They’ve now teamed up with the Hospital for Sick Children (SickKids) to use the technique — MRI-guided focused ultrasound — for a pediatric patient for the first time, delivering chemo to the area near their tumor, as part of a newly launched phase 1 trial.
The moving bubbles temporarily expand the gaps between the cells in the blood-brain barrier, allowing chemo drugs in.
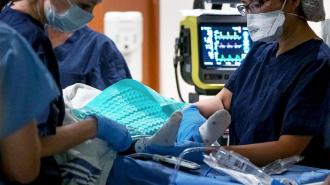
How it works: During MRI-guided focused ultrasound, patients are fitted with a special helmet designed to deliver focused ultrasound waves. They are then placed in an MRI machine so that the doctors can monitor and guide the ultrasound in real time.
While the patient is under general anesthesia, microscopic bubbles — smaller than red blood cells — are injected into their bloodstream. Ultrasound waves from the helmet are used to vibrate the bubbles in the area near the tumor.
The moving bubbles temporarily expand the gaps between the cells in the blood-brain barrier. Intravenously delivered chemotherapy can then slip between the gaps and reach the tumor. Within hours, the gaps in the barrier close again, returning to their pre-treatment size.
Looking ahead: The Canadian researchers expect to enroll 10 children total between the ages of 5 and 18 in their trial. Each will undergo three cycles of chemotherapy, spaced four to six weeks apart.
The purpose of this trial is only to test the safety and feasibility of using MRI-guided focused ultrasound to treat DIPG in children. Larger studies will be needed to determine its efficacy, but if the procedure works as hoped, James Rutka, the study’s co-principal investigator, believes the impact could be life changing.
“It is hoped that these drugs will then act on the tumor cells to obliterate them and to allow for the pons, which is the brain stem, to become normal again and for children to have longer quality of life,” said Rutka.
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].