Stanford researchers have discovered that certain brain signals actually flow the wrong way in people with treatment-resistant depression — and that magnets can correct the misdirection and help patients feel better.
“This is the first time in psychiatry where this particular change in a biology — the flow of signals between these two brain regions — predicts the change in clinical symptoms,” said Nolan Williams, senior author of a paper detailing the discovery.
The challenge: While most people living with depression can find some relief with medications, approximately 84 million people globally have treatment-resistant depression, meaning they still don’t feel better even after trying multiple antidepressants.
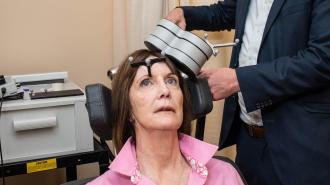
But about 50% of people with treatment-resistant depression do respond to transcranial magnetic stimulation (TMS), according to Adam P. Stern, MD, an assistant professor of psychiatry at Harvard Medical School, who was not involved with the new study. TMS uses magnetic fields to painlessly and noninvasively stimulate nerve cells in the brain, usually for 20-50 minutes a day, five days a week, for several weeks or even months.
“To be honest, I was pretty skeptical.”
Anish Mitra
This has been a life-changing discovery for many people with stubborn depression, but exactly how it works has remained a mystery. That’s made it hard to know which patients are likely to benefit from TMS before they commit to the treatment.
“The leading hypothesis has been that TMS could change the flow of neural activity in the brain,” said Anish Mitra, lead author of the new paper. “But to be honest, I was pretty skeptical.”
What’s new? To test his skepticism, Mitra and his colleagues recruited 33 people with treatment-resistant depression for the study, published in PNAS.
Twenty-three of the participants underwent an accelerated, highly effective version of TMS — known as “Stanford neuromodulation therapy” — that consists of 10 sessions per day for five days. The others received a sham treatment.
All of the participants’ had their brain activity mapped using fMRI before and after the treatment phase of the study. Data was also collected on 85 people without depression.
In 75% of the people with depression, some of the signals flowed the opposite way.
The results: When they analyzed the fMRI data, something stood out: a connection between a brain region that regulates physical sensations (the anterior insula) and a region that governs emotions (the anterior cingulate cortex).
As expected, in the brains of people without depression, signals traveled from the physical sensation area to the emotional area.
“You could think of it as the anterior cingulate cortex receiving this information about the body — like heart rate or temperature — and then deciding how to feel on the basis of all these signals,” explained Mitra.
Within 3 days of finishing the TMS treatment, the reversed signals were flowing in the right direction.
In 75% of the people with depression, however, some of the signals flowed the opposite way, and the more severe a person’s depression, the greater the proportion of wrong-way signals.
“It’s almost as if you’d already decided how you were going to feel, and then everything you were sensing was filtered through that,” said Mitra. “The mood has become primary.”
Within 3 days of finishing the TMS treatment, the reversed signals were flowing in the right direction, and patients were reporting an improvement in their mood — the more severe their depression was to begin with, the greater the reported improvement.
“The technology now is approaching the complexity of the problems we’re trying to understand.”
Mark Raichle
The bottom line: Not everyone with treatment-resistant depression displayed the wrong-way signals, but this finding may turn out to be a useful indicator that a person has depression and is likely to respond to TMS.
“Behavioral conditions like depression have been difficult to capture with imaging because, unlike an obvious brain lesion, they deal with the subtlety of relationships between various parts of the brain,” said senior author Mark Raichle.
“It’s incredibly promising that the technology now is approaching the complexity of the problems we’re trying to understand,” he continued.
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].