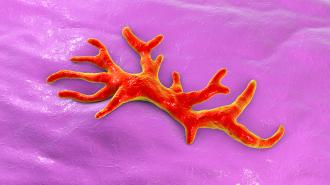
A decades-old drug used to treat urinary tract infections (UTIs) appears to have saved the life of a man infected by the “brain-eating” amoeba — and his case highlights the tremendous potential of a new type of genetic sequencing technology.
The patient: In 2021, a 54-year-old man was admitted to a Northern California hospital following a seizure. After an MRI revealed a mass in his brain, he was transferred to the UCSF Medical Center, where the mass was biopsied.
Based on the biopsy, doctors suspected that the patient’s brain was being attacked by an amoeba — a highly dangerous and unusual infection. They sent a sample to the University of Washington, Seattle, where a PCR test identified the pathogen as Balamuthia mandrillaris — a deadly brain-eating amoeba that kills more than 90% of people it infects.
With the man now showing signs of several brain lesions, the UCSF team started him on an intense regimen of antiparasitic, antibacterial, and antifungal drugs.
“It’s what’s recommended because it was what happened to be used in patients who survived,” Natasha Spottiswoode, leader of the patient’s medical team, told Science Magazine.
After about two weeks, the man’s lesions had shrunk slightly, but he began experiencing severe side effects from the treatment, including kidney failure. The team cut back on his meds, and two weeks later, his lesions were growing again.
Within a week of treatment, his lesions began shrinking, and he was soon discharged.
The drug: While hunting for a new treatment, Spottiswoode came across a 2018 study in which UCSF biochemist Joseph DeRisi screened more than 2,000 compounds in the hope of finding one that would be effective against Balamuthia, which had infected one of his patients.
DeRisi’s team did find one promising candidate — an antibiotic called “nitroxoline” — but the patient succumbed to the brain-eating amoeba before they could use it to treat her.
“I think he’s very much on his way to being one of the survivors of this disease.”
Natasha Spottiswoode
Nitroxoline has been prescribed for UTIs in Europe for about 50 years, but isn’t approved in the US, so Spottiswoode had to reach out to the FDA for permission to administer it to her patient.
Once that was settled, she had to track down the medication — Chinese biotech company Asieris Pharmaceuticals, which is studying its use as a bladder cancer treatment, agreed to provide the pills, pro bono.
The impact: Just over 100 days after he first went to the hospital, the man started taking nitroxoline. Within a week, his lesions began shrinking, and he was soon discharged.
At the time the doctors reported on his case, it had been 15 months since he was initially evaluated, and multiple MRIs post-discharge showed that his lesions are continuing to shrink. He is still taking nitroxoline, but his doctors hope to discontinue it soon.
“I think he’s very much on his way to being one of the survivors of this disease,” Spottiswoode told a group of colleagues in October 2022, according to Science.
The real challenge is diagnosing the infection in the first place.
The big picture: Researchers don’t know how people become infected with Balamuthia, but thankfully, such encounters with the brain-eating amoeba are highly uncommon — about 200 cases have been reported since the pathogen’s discovery in 1986.
Still, the UCSF team has been in talks with the CDC about making sure nitroxoline can be delivered anywhere in the US within 24 hours for those rare cases.
Even then, the real challenge is diagnosing the infection in the first place — had the UCSF team not suspected an amoeba, they wouldn’t have known to order a PCR test to look for amoeba species.
“You let the database match tell you what organisms are in there.”
Michael Wilson
That might not be the case in the future, though, thanks to metagenomic next-generation sequencing (mNGS). This technique can be used to sequence all of the genetic material in a sample at once, and the findings can then be compared to a database on all known pathogens.
“You let the database match tell you what organisms are in there,” Michael Wilson, a neurologist at UCSF, told Science. “You’re not going in with a preconceived notion.”
The technique isn’t yet approved to test brain tissue samples for clinical diagnosis, but after the PCR test came back positive for balamuthia, the UCSF team analyzed a sample from their patient under a research protocol, which confirmed the amoeba’s presence.
The widespread deployment of mNGS could ensure patients get the right treatment right away.
mNGS is still fairly new and has limitations — it costs $2,000 to run the test on a cerebrospinal fluid (CSF) sample at UCSF, and the turnaround time for results can be about a week.
It’s not infallible, either — it missed balamuthia in a CSF sample from the UCSF patient.
If these limitations can be overcome, though, the widespread deployment of mNGS could allow doctors to identify pathogens faster — ensuring patients get the right treatment right away.
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].