The popular weight-loss drug semaglutide reduced patients’ risk of heart attacks, strokes, or death from heart disease by 20%, according to preliminary results of a large trial — a finding that could shake up how the healthcare industry treats obesity.
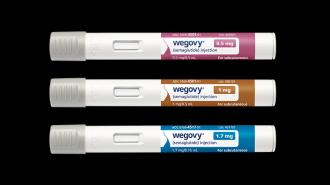
The challenge: Losing weight is notoriously difficult, but for some people, it got easier in 2021, when the FDA approved pharma company Novo Nordisk’s weight-loss drug semaglutide (brand name Wegovy) — in one large trial, people with obesity using the drug lost an average of 12% of their body weight.
Without proof that semaglutide improves heart health, insurers have been reluctant to cover the weight-loss drug.
Being obese or overweight increases the risk of many serious health problems, including diabetes, hypertension, and heart disease, the number one cause of death in America. Losing weight can lower the risk of heart disease — which suggests that semaglutide could improve users’ heart health in addition to helping them shed pounds.
However, without proof of this benefit, private insurers have been reluctant to cover the weight-loss drug. The US government, meanwhile, considers weight-loss treatments “lifestyle drugs” and doesn’t cover them under Medicare.
As a result, many people hoping to use semaglutide to drop weight — for health or aesthetic reasons — have faced the list price, which is $1,350 per month in the US.
What’s new? On August 8, Novo Nordisk announced preliminary results of its phase 3 SELECT trial, which launched in 2018. The trial found that the weight-loss drug reduced the risk of major adverse cardiovascular events (MACEs) — heart attacks, strokes, or cardiovascular deaths — by 20% in people who are overweight or obese, compared to a placebo.
“SELECT is a landmark trial and has demonstrated that semaglutide 2.4 mg has the potential to change how obesity is regarded and treated,” said Martin Holst Lange, executive VP for development at Novo Nordisk.
The risk of MACE in the group that received the weight-loss drug was 20% lower than in the placebo group.
The trial: More than 17,500 people over the age of 45 and diagnosed as either overweight or obese participated in the SELECT trial, which spanned 41 countries. They all had a history of heart disease — either a previous heart attack or stroke, or a diagnosis of symptomatic peripheral arterial disease — but no history of diabetes.
About half of the participants received a 2.4 mg dose of semaglutide, delivered via a pen injection, once per week. The other half injected a placebo. They all received standard care for the prevention of MACEs.
By the end of the study, the risk of MACE in the group that received the weight-loss drug was 20% lower than in the placebo group, meeting the study’s goal of demonstrating a reduction of at least 17%.
The fact that Novo Nordisk chose to focus on people who had already developed cardiovascular disease — which puts them at higher risk of MACE than people who are only overweight or obese — makes this reduction even more notable.
The caveats: Novo Nordisk has only shared the topline results of the trial, so we don’t have many details, and none of the information has undergone peer review yet.
“The obvious conclusion of these findings is that we should view obesity as a medical condition.”
Stephen O’Rahilly
The company didn’t say how long SELECT participants took its weight-loss drug on average, but at the start of the trial, it predicted the average duration would be about 3 to 5 years. To continue to keep the weight off, they’d likely have to take the drug indefinitely — a 2022 study found that people regain most of their lost weight within a year of going off semaglutide.
Additionally, the trial doesn’t tell us how much people with diabetes or those without a history of heart disease would benefit, and while Novo Nordisk says the drug appeared well-tolerated in the trial, the FDA has received reports of people on semaglutide experiencing stomach paralysis.
Looking ahead: Novo Nordisk has said it plans to ask the FDA to update the label for Wegovy to include the reduced risk of cardiovascular events, which could not only encourage more insurance companies to cover the weight-loss drug, but change how the entire healthcare industry approaches obesity.
“The obvious conclusion of these findings is that we should view obesity as a medical condition, like hypertension (high blood pressure), where effective and safe drug therapy can contribute to reducing serious adverse health outcomes,” said Stephen O’Rahilly, head of the University of Cambridge’s department of clinical biochemistry, who wasn’t involved in the trial.
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].