One of the (many) things that has made the coronavirus difficult to contain is the fact that so many people don’t get symptoms until several days after infection — if they get symptoms at all.
More than half of COVID-19 infections may come from “silent transmissions” by these presymptomatic or asymptomatic carriers, who don’t quarantine or get tested because they feel fine.
Now, it turns out that one reason these people don’t feel sick might be because they’re actually getting pain relief from coronavirus — and the discovery could impact not only the pandemic, but the overdose epidemic, too.
Spike Protein, Pain Reliever
Past research has linked certain illnesses, including cancer and arthritis, to a protein called VEGF-A. When this protein binds to another protein, called neuropilin-1, it sets off a domino effect that results in hyper-excited neurons — that’s what causes pain.
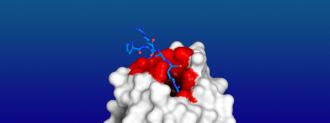
In June, two papers posted on the preprint server bioRXiv suggested that the coronavirus’s spike protein also appears to bind to neuropilin-1, using it as a way to break into the body’s nerve cells. That quickly caught the attention of a group of University of Arizona researchers.
“(F)or the last 15 years, my lab has been studying a complex of proteins and pathways that relate to pain processing that are downstream of neuropilin,” researcher Rajesh Khanna said in a press release, “so we stepped back and realized this could mean that maybe the spike protein is involved in some sort of pain processing.”
Khanna’s team took a closer look at how the spike protein binds to neuropilin-1 and found that it was in exactly the same location as VEGF-A, the pain-triggering protein.
Next, they did a series of lab and rodent experiments to see if it was possible to actually get pain relief from coronavirus.
They first used VEGF-A to hyper-excite neurons and then introduced the spike protein — the neurons immediately returned to their pre-excited state, completely reversing the pain signalling.
“It didn’t matter if we used very high doses of spike or extremely low doses,” Khanna said. “It reversed the pain completely.”
Pain Relief from Coronavirus
Khanna wasn’t kidding when he called the coronavirus “sneaky” in a recent Conversation piece — the virus may be literally tricking people into thinking they don’t have COVID-19 to perpetuate its own spread.
Ultimately, if their immune system defeats the virus, the person may never know they had it. But if the virus isn’t stopped, the damage grows exponentially, triggering a slew of potentially deadly symptoms that cannot be covered up.
But now that we know about this pain relief from coronavirus, we might be able to use it as a weapon against COVID-19 — and (maybe) opioid addiction, too.
We have a pandemic, and we have an opioid epidemic. They’re colliding.
Rajesh Khanna
In terms of the pandemic, researchers could develop drugs that bind to neuropilin-1 first, in the same way the spike protein does. This could block one of the virus’s known entry points into our cells.
Khanna’s team, meanwhile, is already testing the ability of other molecules to bind to neuropilin-1 in a way that mimics the pain relief from coronavirus. If they can identify one that does it effectively and safely, it could become an alternative to potentially addictive opioids for people with chronic pain.
“We have a pandemic, and we have an opioid epidemic. They’re colliding,” Khanna said. “Our findings have massive implications for both.”
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].