There’s a scent of anatomy class in the air.
The steady arms of the new, sterilely wrapped robot — like a spider in a shower cap — move in time with the man at their control console, across the room from his patient.
Pier Giulianotti looks like a phantom organist, with his eyes buried in the console’s view. He’s busy maneuvering the robotic arm as it operates inside the cadaver on the table.
A pallid foot sticks out into view; tissues appear on a large screen showing everyone in the room what Giulianotti, chief of General, Minimally Invasive, and Robotic Surgery at University of Illinois at Chicago Health, sees.
Giulianotti is a pioneer in robotic surgery, his Italian accent and well-tailored suits giving him the air of an orchestra conductor, even when he’s not behind a console. It is his mission to create a world in which the “dream surgery” — one enhanced by digital technology and robotics — is a reality. This reality, according to Guilianotti, would provide for safer, faster, and better surgical procedures.
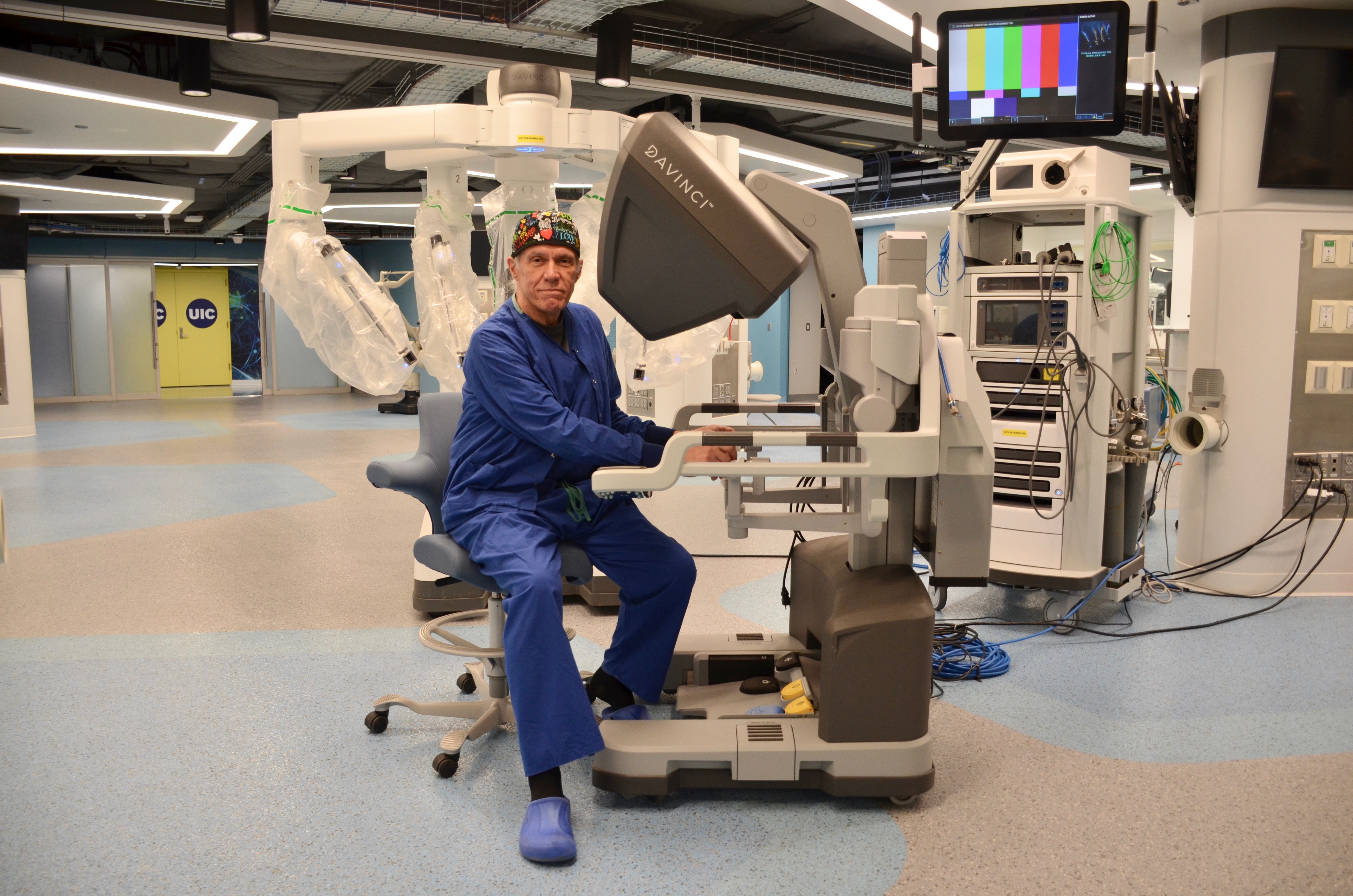
He is hands-on in creating that world right now, testing out a new surgical robot in the Surgical Innovation Training Laboratory (SITL), UIC’s 17,000 square foot facility beneath the streets of the city’s West Side.
Surgical robots are not without their drawbacks, however. Cost can be a challenge, both in acquiring the robots themselves and in training the surgeons to use them. They take time to properly set up, limiting their usefulness in, for example, a battlefield situation.
But advancements in robotic surgeries and towards that digitally-enhanced dream surgery are being made — and Guilianotti and SITL are leading the charge.
Back in the room, I watch quietly as the symphony unfolds.
A Patient’s Digital Twin
Days after I see him operate the robot, I go to Giulianotti’s office, past a mounted copy of his New Yorker profile in the hall.
He punctuates our interview with his body and what’s lying around. He demonstrates stitching on a Kleenex, turning tissue into tissues; he’s tapping his computer tower, a desktop metaphor for the brave new digital dream world of surgery he strives for.
It is virtual reality and the digital world which is the key to Giulianotti’s vision of a perfect, dream operation. While the robots are an innovative tool, they are not the true surgical sea change, he says.
It is instead what they allow.
“With the robots, all the information … in or out, is passing through the computer,” Giulianotti says. The computer perfects and elaborates on the patient and offers this new, better output to him. From here, his skills can be enhanced, he says; he is operating now not inside a body but inside the power of images. (He can be intoxicatingly poetic on this point.)
SITL is currently developing digital twins of patients, highly accurate models built from images of the patient’s body. The end goal is VR simulations so accurate that the surgeon is practically practicing within the patient’s body.
This is the key to Giulianotti’s vision of a dream surgery, and only recently has the computer power been available to create these models.
“To recreate anatomy is certainly not an easy task,” Leo Chen, director of SITL and a biomedical engineering expert, says.
The models are built using CT imaging data. Patients lie down on a CT scanner, a thin bed attached to a large, donut-looking structure. The donut glides down the bed, taking multiple, detailed images from all around the patient, including skeletal structure, organs, and blood vessels.
Advancements towards a digitally-enhanced, robotic dream surgery are being made beneath the streets of Chicago’s West Side.
By combining all of those CT images — different angles, different parts — you end up with a full-body, 3D structure, which is where that computer horsepower comes in.
SITL’s 3D models are currently high-quality enough for surgical planning, Chen says, although they are not full-body. But all the surgeons need is the critical structure, the place being operated on; a 3D model of a tumor and its immediate surroundings, for example.
“Let’s say you have a difficult case,” Giulianotti says. “Planning a difficult surgery. You are getting all the data out of this patient, images, information.” All of that data can be given to an AI, which could give you strategic options; approach this vein from 20°.
“Then, you have a true simulation of the operation.”
A digital twin won’t be teaching your surgeon soon, though.
“For training, that’s still a long way to go,” Chen says. “Because [for] that, you need to almost mimic the human body in every detail.” As computing power increases, this could become a reality — it could one day be possible for surgeons to learn on a full-body model packed with granular detail.
However, digital models are only part of a surgery. Eventually, the blade must meet flesh.
The Vision
“I had a bad family experience,” Giulianotti says, after his morning rounds are done.
“My mom died of ovarian cancer. She went through really bad open surgery, with a lot of suffering and blood loss. I think one day, I had to even give her my blood to help.”
As a surgeon, Giulianotti wants a better way — a way different than what his mother went through.
Giulianotti first saw the robots at a panel summit convened by Johnson & Johnson in the late 1990s, where surgical experts were asked to provide their input on which direction the company should focus its efforts. At the time, laparoscopic surgery, which uses long, narrow instruments and cameras to operate in a minimally invasive way, had completely shifted the field. All surgeries carry risks, and generally speaking, the larger the incision, the higher the risk. As laparoscopy reduced the amount of surgeries that required opening patients wide, safer, better tolerated surgery led to better outcomes.
He saw robotic surgery as the next major step.
The Robots
Intuitive’s da Vinci surgical robot system currently dominates the market. It includes the control panel, a vision cart, and the patient cart — what you’d think of as the robot per se. From a central trunk extend multiple arms. These arms include a camera system and an array of swappable surgical tools.
Generally, robotic surgery can provide patients with better outcomes; less blood loss, less pain, and quicker recoveries, Jihad Kaouk, at Cleveland Clinic’s Glickman Urological & Kidney Institute tells me. Kaouk is the director of the Center of Advanced Robotic and Image Guided Surgery. Although UC Davis assistant professor of clinical surgery Victoria Lyo tells me there’s not yet enough data to say robots are superior to laparoscopy, general consensus is that they are beneficial.
The robots allow for difficult-to-operate-on places, like the prostate, to be more safely and easily accessed.
Using detailed digital models of the patient, surgeons could game plan for and practice procedures with a level of personalized precision impossible before.
“The anatomical location of the prostate, deep in the pelvis, with the pubic bone and the shadow, makes it very hard to see in the pelvis and perform surgery open,” Kaouk says, referring to the traditional method of, well, opening a person up.
In some cases, the surgical robots allow for surgeries that would have previously never happened. When a kidney transplant patient is too obese, they no longer can safely go through the procedure. Cruelly, patients with obesity often have type 2 diabetes, a predominant cause of chronic kidney disease. These patients are more difficult to work on, and tend to have worse outcomes.
But robotic kidney transplantation involves smaller incisions and better visualization thanks to their camera, so patients that previously would have been ineligible to receive their new kidneys can get one, Patrick Dean, surgical director of the Mayo Clinic’s kidney transplant program, tells me.
Eventually, the robots may perform these surgeries on their own.
In one corner of the lab, an older da Vinci robot is hooked to a computer. By feeding hours and hours of surgery footage to a machine learning AI, the lab is attempting to develop a completely autonomous surgeon. Chen imagines that an AI would first act as something of an assistant, using computer vision to help warn surgeons of blood vessels they can’t see, perhaps, or helping to determine the accuracy of their cuts.
The next step could be the automation of certain aspects of surgery; internal suture, perhaps, which could potentially be done much more quickly and accurately by machine, poppoppoppop, or first incisions, guaranteed to be in the right place at the correct depth. Giulianotti predicts AI will be operating on you within a decade, or perhaps 15 years — a physical manifestation of digital surgery.
Giulianotti wants to create a new world where the digitally-enhanced dream operation means less blood, less infection, less risk, scarring, and pain.
The Dream
Less infection, less blood loss; less risk, less scarring; less pain. AI-powered models would let surgeons develop custom plans of action, to be carried out with AI-assisted confidence using robots capable of enhancing a surgeon’s abilities to something approaching superhuman — this is Giulianotti’s dream.
He wants to create new digital senses — perhaps filters to see dyes, to see blood flowing, neurons firing, targets to hit, traps to avoid, to allow human vision to supersede the eye. He wants to create a new world where the dream operation can become a reality, SITL its womb.
“Can we do that as humans?” he asks.
“No.”
But humans — along with digital models, and robots — can.
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].






