“In general, there has been more hype around AI in health care than meaningful results.” That was Michael Dowling, the CEO of Northwell Health, and Charles Kenny, executive editor of the Northwell Series on Health Care Innovation, back in 2018, in their book Health Care Reboot.
They elaborated: “While telehealth is up and running and very real, AI remains in its early stages. But the possibilities are such that there is much excitement about a future in which smart computers require only seconds to make a complex diagnosis and prescribe a treatment plan.”
Fast forward to the present, and while the hype still outpaces reality, the contours of those possibilities are beginning to take shape. Research teams are busy developing machine-learning models that can help doctors make diagnoses at a fraction of the time and cost it would take a human practitioner. One such AI aims to help doctors predict patients’ risk of developing serious cardiovascular conditions later in life — and the initial results are promising.
The heart of the matter
Cardiovascular diseases are the leading cause of death in the United States. In 2021, roughly 695,000 Americans died from heart disease. That’s about 1 in every 5 deaths nationwide. Globally, the death toll is even more stark. Such diseases claim an estimated 17.9 million people per year — a third of all deaths.
Doctors have many methods to predict the likelihood a patient will develop cardiovascular diseases. One such predictor is called “abdominal aortic calcification” (AAC).
The abdominal aorta is the body’s largest blood vessel. About the width of a garden hose, it runs from the heart down to the abdomen, and like any blood vessel, plaque can build up in it over time. This plaque contains calcium that can harden into crystals along the vessel wall — a process known as “calcification” or, more commonly, the “hardening of the arteries.”
This process happens slowly over decades, and often by the time someone is diagnosed with heart disease, a considerable amount of damage has already been done. If doctors can detect this calcification early, they can warn their patients and advise them on how to reduce their risk of a heart attack or stroke later in life.
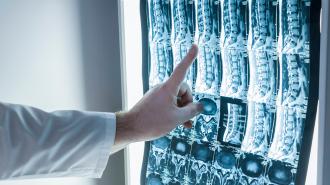
Thankfully, measuring a patient’s AAC doesn’t require an invasive or overly expensive test. A simple X-ray will suffice, the same kind routinely used to detect osteoporosis in fact. When an X-ray is taken of a patient’s lower back, a specialist can visually measure the calcification in the patient’s abdominal aorta and plug those measurements into a scoring system. The higher the score, the more calcification, the greater the risk.
And research shows this test works. A 2021 meta-analysis of observational studies found “moderate to high-quality evidence” that advanced AAC substantially increased both a patient’s absolute and relative risk of cardiovascular disease and all-cause mortality. The authors further note that AAC detection was an “underappreciated measure” for prevention and management strategies, especially for “people with substantially higher risk of clinical cardiovascular events and poorer long-term prognosis.”
An instant prognosis
There is, however, a rub. While X-rays that can detect AAC are common, they require trained specialists to analyze and score the images. That process is expensive and time-consuming.
Enter AI. A team of researchers out of Edith Cowan University developed a neural network to analyze X-ray images for AAC build-up. After training, the neural network algorithm underwent a validation test on a dataset of about 5,000 images taken from real-world checkups. Its scores were compared with those separately provided by imaging specialists to determine accuracy.
The results showed that the AI arrived at the same score as the specialist — low, moderate, or high AAC — around 80% of the time. The AI did incorrectly diagnose some people with having high AAC when they actually had low AAC; however, that mistake only occurred 3% of the time. Joshua Lewis, the study’s principal investigator and a Heart Foundation Future Leader fellow, called the results impressive for version 1.0 of the system while noting that there was room for improvement.
“Automated assessment of the presence and extent of AAC with similar accuracy to imaging specialists provides the possibility of large-scale screening for cardiovascular disease and other conditions — even before someone has any symptoms,” Lewis said in a press release.
“This will allow people at risk to make the necessary lifestyle changes far earlier and put them in a better place to be healthier in their later years,” he added.
Importantly, the AI worked remarkably fast. According to the release, it takes a human specialist anywhere from 5-15 minutes to analyze a single image. At that rate, a human could potentially perform as many as 500 analyses a day (if they are really cranking them out). Conversely, the AI can scan such images at a blistering speed of 60,000 images a day.
“Since these images and automated scores can be rapidly and easily acquired at the time of bone density testing, this may lead to new approaches in the future for early cardiovascular disease detection and disease monitoring during routine clinical practice,” Lewis said.
The research was published in eBioMedicine, a peer-reviewed, open-access medical journal published by The Lancet.
This will allow people at risk to make the necessary lifestyle changes far earlier and put them in a better place to be healthier in their later years
Joshua Lewis, Heart Foundation Future Leader fellow
Small changes, outsized impacts?
This AI is one of a multitude in development that might one day help doctors predict patients’ risk of developing various diseases. Other teams have been hard at work developing programs to diagnose breast and pancreatic cancer, as well as other methods for diagnosing various forms of heart disease. Each one could serve as an initial screening and help people understand their risk before they start having symptoms.
We’re still a long way off from the dream of an AI that can make complex diagnoses and prescribe treatments for a range of diseases without a human backing it up — if that day comes at all. However, bespoke AI may soon help speed up routine processes, quickly manage backlogs, and give doctors more time to spend with patients instead of screens. All of which may be more valuable in the long run — and more realistic in the short.
As Dowling and Kenny pointed out years ago: “Sometimes the simplest technologies can make a significant difference in patient care.”