This article is an installment of The Future Explored, a weekly guide to world-changing technology. You can get stories like this one straight to your inbox every Thursday morning by subscribing here.
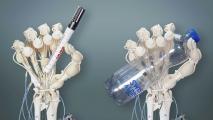
Scientists are printing tiny human organs — thousands per hour — to test new drugs that could treat COVID-19.
Why this matters: Testing new drugs can be a pretty lengthy process — on average, it takes 10 years and $2.6 billion. Typically, scientists have to study the drug in petri dishes and lab rats before they can even try it on human beings. (Only 1 in 1,000 drugs ever make it out of the lab into human trials.) While this can help ensure safety, it can also be time-consuming. And time is precious — especially in the midst of a pandemic.
Tiny human organs made in labs, however, offer scientists a way to skip the animal trials and go straight to studying the drugs on actual human tissue — potentially giving patients quicker access to new, life-saving treatments.
Printing thousands of mini-organs means we could run big, statistically significant drug trials — just for you — on multiple different treatment options.
Personalized medicine beyond COVID-19: Mini-organs could also usher in a new era of personalized medicine. Human beings are unique — and drugs often react differently in different people. But if scientists could print a replica of your organ (or, say, tumor), they could see if a certain medication would be effective for your particular health issue. And if they could print thousands of these mini-me organs, they could run big, statistically significant drug trials — just for you — potentially on multiple different treatment options.
Scientists are also hopeful that these replicas could eventually be placed inside a person, eliminating the need for organ donors. Since the replicas could be made from the person’s own cells, organ rejection (when the recipients’ immune system sees the new organ as a foreign invader and tries to attack it) wouldn’t be a problem. It could also be used to grow new skin, crucial for burn victims, bone, cartilage, and even blood vessels.
How it works: Bioprinting, the method for printing these organs, is similar to 3D printing — but instead of plastic or metal, scientists use stem cells and other biological materials that (when encapsulated in a “hydrogel”) act as the “ink.”
Like any kind of printing, you’ll need something to print the bioink on — and in this case, grow on. The foundation for bioprinting is usually a scaffold made of biodegradable materials. The bioink is then printed onto the scaffold layer by layer — like a cake!
No surgery required: Usually, getting anything inside a patient requires invasive surgery. But a recent study suggests maybe not so much for bioprinted body parts. An international team of scientists created a bioink from cartilage cells, which they then injected under the skin of mice. Using near-infrared light and clever genetic engineering, scientists were able to deliver instructions to the cells, ordering them to grow into ears — all without needing to make an incision. (Yeah, kinda weird and creepy on mice, but potentially useful for humans who need ear repair.)
Infecting mini-organs with COVID: We still don’t know much about COVID-19’s effects on specific organs — but several research groups are hoping these mini-organs can provide us with better insight. Researchers in Boston are infecting mini-lungs to study the body’s reaction to the disease — hoping to understand why COVID-19 kills some patients and not others. In May, an international research team used mini-organs to understand how blood vessels and kidneys are affected. A team at Wake Forest is also creating mini-lungs — as well as mini-colons — to test novel treatments.
Challenges: The holy-grail for these mini-organs is to be able to bioprint them on demand for use inside a human body — and we’re still years away from that. The human body is extremely complex and being able to replicate it with precision poses lots of challenges — for one, the printers will have to get much faster and more accurate if scientists want to scale up this process for medical use. Two, we’re not sure if these printed structures will be able to retain their structure over time once implanted into the body — plus, some of the scaffolding materials currently used could provoke an immune response from the body. There’s also limited options for bioink materials — scientists have to have just the right blend of materials that are both degradable and don’t pose a health problem but are also strong enough to maintain structural integrity.
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].