Psychedelic-assisted therapy is now officially legal in Canada — for some people.
Starting on January 5, Health Canada — northern counterpart to the FDA — activated amendments to the country’s Special Access Program (SAP). The new amendments “permit physicians to request access to psychedelics for eligible patients,” the Canadian business law firm McMillan explains.
The amendments allow for manufacturers of psychedelic compounds to provide drugs to medical professionals whose patients meet Health Canada’s criteria of having a life-threatening condition resistant to other treatments — or that they believe would require a treatment not available in the Great White North.
“It’s a seismic shift in the level of legalization in Canada…. They’ve been shifted from an illegal drug to a prescribable medicine,” David Harder, operator of psychedelic therapy provider ATMA Calgary Urban Journey Centre told the Calgary Herald.
Combined with therapy and given in clinical settings, psychedelics have shown strong potential to treat depression, PTSD, and other tough to treat disorders.
Psychedelic potential: After decades of draconian drug policies and research labs going dark, psychedelics have entered their research renaissance — and are even turning the corner from academic field to clinical industry.
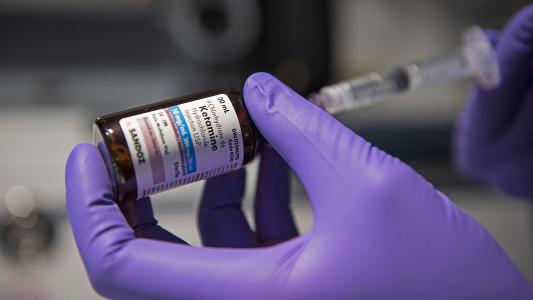
When combined with therapy and given in clinical settings, drugs like ketamine and psilocybin have shown promising potential as antidepressants, while MDMA looks to be an effective therapeutic for PTSD, a particularly difficult to treat disorder.
A new level of access: Canadians could theoretically access psychedelics before now, but they were granted on an individual basis for palliative care.
“I had to write all these letters telling the government why I needed the drugs while doing chemo. It was exhausting,” Laurie Brooks, a terminal cancer patient, told the Vancouver Sun about her experiences seeking psychedelic-assisted therapy under the previous rules.
Under the new amendment, medical practitioners will put in applications to the SAP for their patients. The program aims to have responses for each patient available in days, and there is no waitlist, the Sun reports. The drugs will have to be given in clinical settings.
The new amendment allows doctors to put in applications for their patients. If approved, they can prescribe them psychedelics.
Still, challenges to accessing psychedelic therapy remain. Mental health practitioners and physicians will need to be better trained, Michael Verbora, the medical director of psychedelic therapy provider Field Trip Health, told the Canadian Press.
Field Trip co-founder Ronan Levy told the Press that he still believes most patients will have their applications rejected, with only the most severe cases getting accepted. He hopes that the criteria will loosen in the future.
We’d love to hear from you! If you have a comment about this article or if you have a tip for a future Freethink story, please email us at [email protected].